The COVID-19 pandemic highlighted major issues in the ways the health care workforce in the United States withstands shocks. Staffing issues put nurses in the headlines. In reaction to the public health emergency, all governors issued executive orders to allow nurses to work across state lines more freely. This action was a nationalization of an existing compact between many states. Those emergency orders have since expired, leaving room for policy interventions that can make labor markets more flexible and benefit workers.
In this post, we summarize changes to licensing requirements for nurses from before and during the pandemic, focusing on the Nurse Licensure Compact (NLC) and its reforms to interstate licensing. We provide evidence on both the benefits and consequences of licensing changes and outline the current debate surrounding these reforms. We also provide an overview of the current landscape of nurse licensing in the United States and conclude by considering the future of these reforms in four states that do not currently belong to the NLC.
The Introduction and Expansion of the Nurse Licensure Compact
The Nurse Licensure Compact (NLC) has grown since its inception in 1999. The compact increases the mobility of nurses nationwide by minimizing barriers to interstate practice. Prior to its implementation, nurses had to be licensed to work state-by-state, creating barriers to geographic mobility and interstate work. In the late 1990s, the National Council of State Boards of Nursing (NCSBN) explored a “mutual recognition model” between participating states for licensing of registered nurses (RNs) and practical/vocational nurses (LPN/VNs). This would allow in-person and virtual practice in participating states and would allow nurses to relocate to participating states without relicensing.
In 1997 the NCSBN unanimously endorsed a new model for nursing regulation, laying the foundation for the NLC to be ratified in 1999. Compact membership required Boards of Nursing to report to the newly formed Interstate Commission of Nurse Licensure Compact Administrators (ICNLCA), cease collecting licensing fees from nurses in other compact states, and pay a $6,000 annual membership fee.
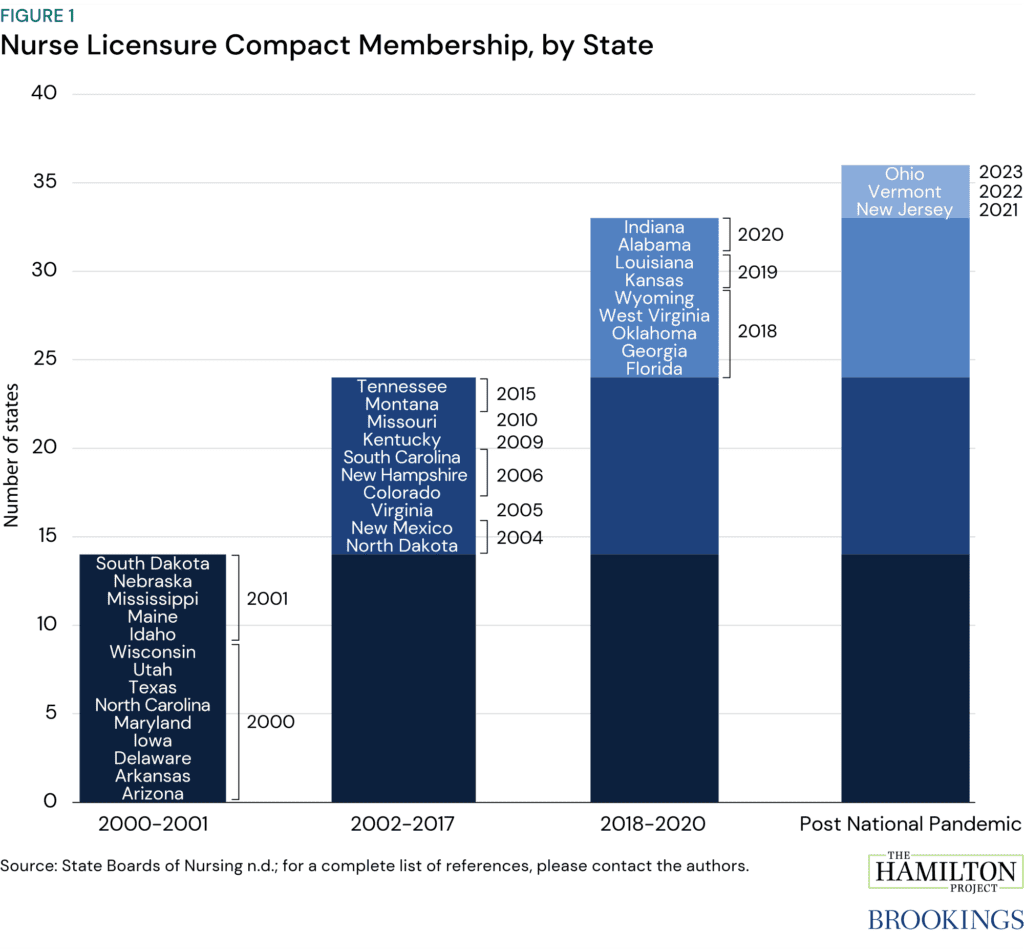
Figure 1 shows the timing of the Nurse Licensing Compact adoption across states. The bulk of adoption took place in the first two years of the compact: 2000-2001. This amounted to 14 states. In the next 15 years, by comparison, 11 states joined the compact. Some attribute this plateau in new membership to the compact’s insufficient criminal background check requirements. On January 19, 2018, the Enhanced Nursing Licensure Compact (eNLC) was formed to address these concerns through 11 new uniform licensing requirements, aiming to encourage its national adoption. In the following two years, 9 more states joined the eNLC, and all previous member states were grandfathered into the new compact. One exception, Rhode Island, joined the NLC in 2008 but opted not to join the eNLC in 2018. After the incidence of the national pandemic which introduced the State of Emergency quasi-national compact discussed below, 3 more states joined the eNLC, the most recent of which is Ohio, joining the compact on January 1, 2023.
Evidence of the Effects of the Nurse Licensing Compact
Just prior to the pandemic, interstate nursing practice was becoming more common in eNLC states. Multi-state licensure take-up has been steadily increasing from 1.6 percent of NLC nurses working in a compact state in 2008, to almost a quarter of all RNs holding an interstate license (24 percent) by 2020. Thirty-three percent of nurses cite using their interstate license for travel nursing, with 16 percent for telehealth and 8 percent for distance education, yet only 4 percent cite travel nursing as their main motivation for obtaining this license.
The literature largely corroborates the causal impact of compact membership on greater mobility among nurses. Shakya, Ghosh, and Norris exploit the diversity in states’ timing of NLC adoption, calculating that compact nurses are 11 percent more likely to move and work in other compact states. Ghani finds that the single-state licensing system causes more rigidity in the labor market, whereas the NLC boosts interstate migration and might divert flows toward non-compact states. Moreover, Johnson and Kleiners’ report on labor migration patterns shows that the NLC both boosts job outflows within the health and social assistance industry by 11 percent and dampens the number of health workers moving from compact to non-compact states. Conversely, DePasquale and Stange’s research on commuting found no causal effects on labor supply or mobility; nurses living in a metropolitan statistical area that spans multiple states experience only a 1.2 percent increase in likelihood of interstate work after their state joins the NLC. research on commuting found no causal effects on labor supply or mobility; nurses living in a metropolitan statistical area that spans multiple states experience only a 1.2 percent increase in likelihood of interstate work after their state joins the NLC.
COVID-19 and the Emergency Licensing Waiver: A Quasi-National Compact
The outbreak of COVID-19 prompted all states to declare a State of Emergency in 2020 and implement an emergency licensing waiver for health care professionals, initiating a functionally national compact to make labor markets more flexible. Nurses could effectively practice anywhere without applying for an additional license or paying additional fees, regardless of a state’s pre-pandemic membership in the compact. In analyzing the impact of COVID-19 on the active nursing population, Chan and collaborators claim that “at no other time in the history of the United States has the NLC been more critical for nurse licensure regulation than the COVID-19 pandemic.”
There was an estimated 35 percent growth of travel nursing in 2020 and an additional 40 percent growth in 2021. Wages for those willing to travel skyrocketed to an average of $154 an hour, not including other cash incentives. For nurses willing to relocate on a more permanent basis, signing bonuses reached as high as $13,000.

States began rescinding their states of emergency as early as April 2021, and the majority of states allowed their temporary emergency authorizations to expire by September 2022. Figure 2 shows the timing of exit from the quasi-national emergency compact. States in solid colors exited the national compact into the existing eNLC while states with horizontal lines reverted to nonparticipation in the eNLC. To be clear, however, the historically tight labor market during the recovery from the pandemic has likely been—and continues to be—more consequential to the nursing labor market than changes to licensing.
The Debate Surrounding the Nursing License Compact
Many states have reconsidered NLC membership following temporary measures implemented over the pandemic as possible solutions to labor shortages and turnover. The Massachusetts State Legislature has recently considered joining the eNLC. As of February 2023, Bill H.1284 sits with the Joint Committee on Health Care Financing, bolstered by support from the Massachusetts Health and Hospital Association. During the pandemic, the state’s declaration of emergency permitted out-of-state licensed health professionals to practice in Massachusetts through June 30, 2023. By May 2021, the Board of Registration in Nursing had issued 8,500 temporary licenses. Washington state is also considering joining the compact, with both House Bill 1417 and Senate Bill 5499 in committee as of February 2023. Illinois is reconsidering its licensing practices in the face of looming shortages as well. In response to the public health emergency in early 2020, Governor J. B. Pritzker signed multiple executive orders to allow temporary nursing assistants to perform the tasks typically completed by certified nursing assistants. Out-of-state nurses could also complete the Health Care Temporary Practice Application to receive a temporary Illinois permit. The ability to practice with a temporary permit expired in February 2023.
While participating in the common market may help to alleviate nursing shortages, for a variety of reasons some states pursue a more limited strategy. For example, California and Oregon have considered joining the compact several times. Opposition to NLC implementation from Boards of Nursing have cited concerns over falling nursing board revenues and work standards, a lack of disciplinary oversight, and a loss of sovereignty to the ICNLCA. Some nursing advocacy organizations and affiliated unions highlight worries over diminished bargaining power, as well as wage depression caused by an influx of traveling nurses. If, for example, the removal of licensing restrictions encourages nurses to travel to a state that enjoys elevated wages, then unionized nurses may suffer from declining wages, erasing the above-average wages that the state boasted before joining the compact.
In California, the state of emergency permitted out-of-state nurses to practice without a California-issued license, but authorization expires at the end of February 2023. Oregon has also considered joining the NLC in the past but abandoned this effort in 2016 after facing opposition from the Oregon Nurse’s Association. Temporary emergency licenses for out-of-state nurses were allowed under Governor Kate Brown’s March 2020 emergency declaration; those with such licenses could practice until mid-2023. Oregon’s Nursing Board reports over 11,000 emergency authorizations issued over the two years, and as of June 2022, about one-third of the 9,000 active authorizations had applied for and received an Oregon state license to practice after the state of emergency expired.
Conclusion
States participating in a compact enjoy higher mobility and more interstate practice, with some uncertainty over the magnitude of these impacts. Supporters of the NLC have long envisioned a scaling up of those benefits through a standardized national framework for licensure reciprocity.
The pandemic and concurrent changes to occupational licensing highlighted the need for policy interventions that can benefit workers. Working conditions and burnout have worsened, perhaps exacerbated by significant workforce changes as more nurses temporarily moved across state lines. In addition, turnover and the impending wave of retirements may change post-pandemic workforce projections for nursing. While the current compact focuses on the standardization of state nursing licenses for in-person medical care, the rise of remote medical services before and during the pandemic presents a new challenge to individual state systems, where barriers remain to offering interstate telehealth services.
The flexibility provided to nurses during the pandemic, both in the model of the NLC allowing nurses to move to places of high demand, as well as the easing of requirements around remote medical care, represent possible reforms. In light of changing demographics and geographic disparities in health care access, the need is evident for more flexibility in the structure of medical licensing and provision of care alongside policies that improve working conditions.
Acknowledgments: The authors thank Wendy Edelberg, Ryan Nunn, and Marie Wilken for substantial feedback on this piece and Lucas Fox, Isabel Leigh, and Noadia Steinmetz-Silber for research assistance.




